
Hi {{ first name | there}},
Last week's poll gave us a useful signal from your responses: the biggest friction point was keeping bedtime consistent (26.3%), followed by tracking for 7 days and stopping calories 3 hours before bed (both 21.1%). This week is about the same core tension: how to improve health when your schedule and biology do not always cooperate.
This issue is for the people who keep hearing "just sleep earlier" and thinking, "That is not how my life works."
If this week's newsletter helps, forward it to one smart night owl who needs a realistic plan, not another moral lecture about the 5 a.m. club. Subscribe here.
Evidence-first health, delivered – and built. (And yes, this kind of weekly scoreboard is exactly the kind of thing we are building into HEALTH HACK Pro.)
-LONGEVITY PLAYBOOK-
Night Owls Need a Different Heart-Health Playbook

A new prospective study in UK Biobank (published in the Journal of the American Heart Association) found that people with an evening chronotype had a modestly higher cardiovascular disease risk, but the important part is this: the association was mainly explained by poorer overall cardiovascular health (Life's Essential 8), not an unavoidable "night owl fate." In the paper, LE8 explained most of the association for evening chronotype, and the authors explicitly conclude that evening chronotypes may benefit from interventions targeting cardiovascular risk factors.
This is a very HEALTH HACK finding because it moves the conversation away from identity ("I am a night owl") and toward decision rules ("What do I change first that actually moves risk?"). The study does not prove that changing your habits will erase all risk, but it strongly supports a practical framing: focus on the behaviors that cluster around late schedules, not just the label.
Why now
We just spent a week talking about sleep-aligned meal timing. This is the next layer: what if your real problem is not one dinner, but a recurring pattern of circadian friction (late light, late eating, less consistent sleep, more nicotine/alcohol exposure, less morning light, less routine)? The American Heart Association's 2025 scientific statement is very clear that circadian health affects cardiometabolic function and highlights timing of light, meals, exercise, and sleep as modifiable synchronizers.
Mechanism – simplified
You do not need to memorize clock genes to use this.
The useful model is:
Chronotype = your natural timing preference
Circadian misalignment = when your real life repeatedly fights that timing (or pushes it later while society still expects early performance)
Risk often shows up through behavior patterns and physiological spillover:
less consistent sleep timing
late light exposure
late eating
worse nicotine/alcohol patterns in some groups
poorer blood pressure and metabolic regulation over time
That is exactly why the JAHA paper is so actionable: it points to modifiable CVD risk factors, not just a personality trait.
Reality check
This was a large prospective cohort, not a randomized trial. Chronotype was self-reported, and observational mediation analyses are useful for strategy but cannot prove a single causal pathway. Also, the result is about risk over time, not "your heart is damaged because you stayed up late this week."
It also does not mean every night owl should force a morning-lark life. For many readers, the win is not becoming a different species. It is reducing circadian friction and tightening a few high-yield habits that carry most of the risk signal.
Who this does not directly apply to: shift workers with rotating schedules (different physiology + constraints), people with untreated sleep apnea, and people with suspected bipolar spectrum disorders where aggressive sleep schedule changes can backfire. (Those situations need more individualized clinical guidance.)
THE PROTOCOL
14-Day Night Owl Damage-Control Sprint
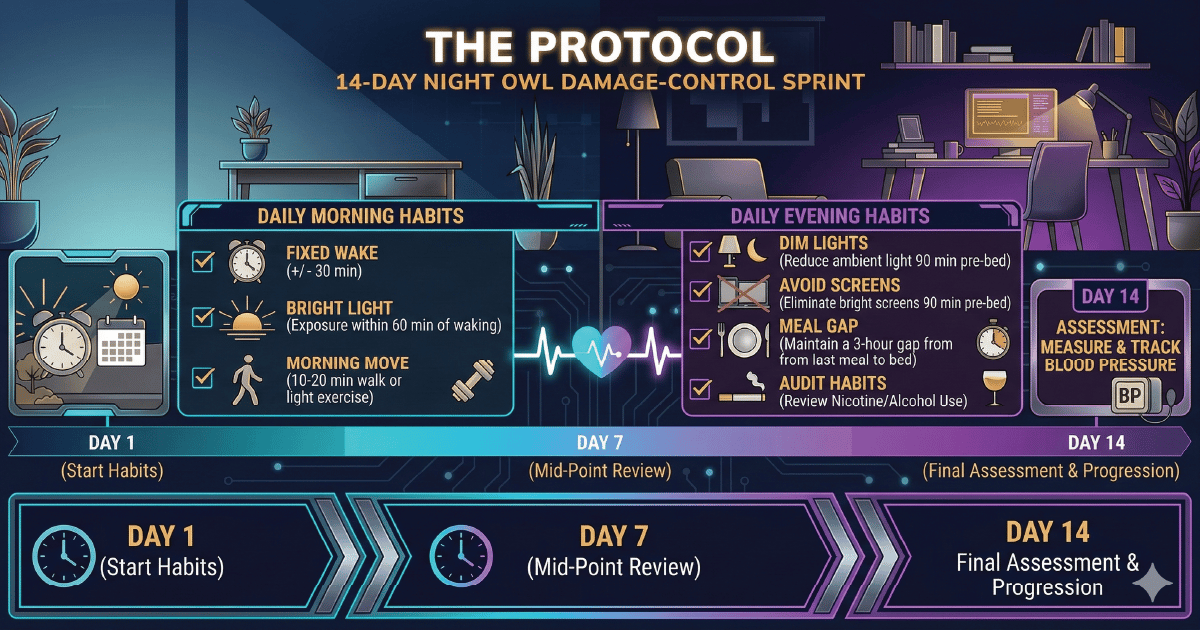
This is a risk-reduction experiment, not a personality conversion campaign.
Step-by-step
Pick a fixed wake time (the anchor)
Keep it within +/-30 minutes for 14 days, including weekends if possible.
Get bright light within 60 minutes of waking
Best: outdoor light.
Backup: a bright-light box if outdoor light is not practical.
Set one movement anchor in your first half of day
10–20 minutes walk, or
short strength/mobility session
Keep it boring and repeatable.
Create a "late-light friction rule"
For the last 90 minutes before bed:
dim room lights
avoid "full-brightness face light" (phone in bed, overheads, etc.)
Keep the 3-hour meal-to-bed gap on at least 4 nights/week
You do not need perfection to get signal.
Run a nicotine/alcohol audit (honest, not performative)
Did either one move later into the evening this week?
If yes, mark it. Do not rationalize it.
Measure blood pressure the same way, on the same days
We are looking for trend quality, not one hero reading.
Measurement instructions (simple, standardized)
Track these for 14 days:
Wake time
"Light within 60 minutes" (yes/no)
Last calories to bed gap (hours)
Bedtime
Morning home BP (on 4–7 mornings/week)
Morning energy (1–10)
How to measure BP (keep the signal clean):
no caffeine/exercise/smoking for ~30 minutes before
sit quietly for 5 minutes
back supported, feet flat, legs uncrossed
cuff on bare upper arm at heart level
take 2 readings (1 minute apart) and log them
measure around the same time each day
This is consistent with AHA home BP measurement guidance and the AHA/AMA policy statement on self-measured BP monitoring.
Safety line (read this)
Do not run this as written if you are a rotating shift worker, pregnant, have a history of mania/hypomania triggered by sleep changes, or have an eating disorder history. Stop and seek care if you get chest pain, fainting, severe shortness of breath, severe palpitations, or concerning blood pressure readings (especially with symptoms).
TINY SCOREBOARD
Reply and paste this in:
Wake-time consistency (days within +/-30 min): __ / 14
Morning light within 60 min: __ / 14
Last calories >=3 hours before bed: __ / 14
BP average (days 1–3): __ / __ mmHg
BP average (days 12–14): __ / __ mmHg
Morning energy (avg, 1–10): __
What broke the streak most often: __
-BIOMARKER OF THE WEEK-
Home blood pressure (morning average)
What it is:
A repeatable, out-of-office measure of your blood pressure taken at home under standardized conditions. For this issue, we care less about a single number and more about the trend across days.
How to measure:
Use a validated upper-arm cuff and the same routine each time (same time of day, seated, rested, two readings). AHA guidance and the AHA/AMA policy statement both support self-measured BP as a validated out-of-office approach.
What "better" generally means:
For this 14-day experiment, "better" means:
readings collected consistently
a stable or improving average over time
fewer obvious spikes tied to bad sleep / alcohol / late meals
Do not overreact to one off-day reading.
Why it matters:
Out-of-office BP is not just a convenience metric. It is clinically useful for diagnosis/management context and can reveal patterns missed by office-only readings (including masked and morning hypertension).
-MYTH OF THE WEEK-
"If I am a night owl, my heart risk is basically fixed."
Why this is wrong:
The new JAHA UK Biobank analysis is almost the opposite message. Evening chronotype was linked to modestly higher CVD risk, but the association was largely explained by overall cardiovascular health (LE8). Translation: the risk signal appears to travel through modifiable behaviors and risk factors, not just a fixed identity label.
Safer replacement behavior (actionable):
Stop trying to "become a morning person" overnight. Start with this sequence:
fixed wake time
morning light
late-light reduction
BP tracking
That sequence respects biology better than willpower theater.
THE "SUPPLEMENT"
Bright morning light (outdoor light first, light box if needed)

This week's "supplement" is not a pill. It is timed light.
What it is
Bright light in the morning is one of the strongest external timing signals ("zeitgebers") for the circadian system. The AHA scientific statement explicitly highlights morning bright light exposure and avoiding light at night as strategies to improve circadian health and reduce disruption.
Evidence summary (why it matters here)
We are not using morning light as a magic cure.
We are using it as a clock-alignment tool for people whose schedules drift later.
A systematic review in delayed sleep-wake phase disorder suggests light therapy can help advance sleep timing in at least some contexts, though protocols vary and the evidence is not fully conclusive.
Light therapy for the treatment of delayed sleep-wake phase disorder in adults: a systematic reviewA new 2026 Scientific Reports study in adolescents also reinforces an important nuance: late evening room light + sleep restriction can blunt the phase-advancing effect of bright morning light. In plain English: morning light helps, but it works worse if you keep blasting yourself with late light and cutting sleep.
Late evening room light and sleep restriction reduces the ability of bright morning light to phase advance adolescents’ circadian clocks
Practical use framing (keep it boring and doable)
Best option: Get outdoor light in your eyes (not staring at the sun) within 60 minutes of waking.
If not possible: Use a bright-light box while reading/planning breakfast.
Keep this paired with your fixed wake time. Light without timing consistency is weaker.
Safety / contraindications
If you have bipolar disorder, retinal disease, severe migraines triggered by light, or you are on photosensitizing meds, discuss light therapy devices with a clinician before using them. If a light box worsens agitation, headaches, or sleep, stop.
-IN THE PRESS-
What we're reading
Can Lithium Protect the Aging Brain?
A pilot RCT (LATTICE) tested low-dose lithium in mild cognitive impairment for 2 years: none of the 6 coprimary outcomes hit the prespecified significance threshold, but verbal memory decline looked directionally better. Interesting signal, not a green light – lithium is prescription-grade and monitoring-heavy.
MedPage Today
Physical Activity and Early Rising Linked to Lower ALS Risk
This one fits the theme: an AAN meeting report suggests morning chronotype and regular activity are associated with lower ALS risk. Reality check: it is preliminary conference data and observational – compelling for hypothesis, not causality.
Neuroscience News
Superagers' 'Secret Ingredient' May Be The Growth of New Brain Cells
A high-quality "superager" angle: a Nature paper uses multi-omics on human hippocampal tissue and asks what neurogenesis looks like in people with exceptional memory aging. Cool biology – but it is still correlational and not a DIY "boost neurogenesis" play.
ScienceAlert
A ketogenic diet enhances aerobic exercise adaptation and promotes muscle mitochondrial remodeling in hyperglycemic male mice
In hyperglycemic male mice, a ketogenic diet lowered glucose and restored VO2peak training adaptation – suggesting "metabolic context" can gate training response. Important limitation: mouse model, plus ketogenic diets can trade endurance feel/performance for metabolic shifts depending on context.
Nature Communications
Lab-Grown Brains Growing More Powerful
Organoids got trained on a classic control task (cart-pole) via feedback – a step toward "adaptive organoid computation." Fascinating, ethically loaded, and mostly a reminder that neuroscience is moving faster than our intuitions about what counts as "learning."
Futurism
-PEPTIDE OF THE WEEK-
Elamipretide / SS-31 (mitochondria-targeting tetrapeptide drug)
The mitochondrial promise – and the evidence gap

Elamipretide (also known as SS-31; brand name Forzinity for one approved indication) is one of the rare peptides that sits in a very different category than influencer-grade "recovery peptides." It has real drug-development history, real clinical trials, and a real FDA approval. That makes it more interesting.
It also makes it easier to misuse in conversation.
The promise is obvious: a peptide that targets mitochondrial dysfunction by interacting with cardiolipin in the inner mitochondrial membrane sounds like a "longevity shortcut." The evidence gap is just as important: the strongest clinical/regulatory evidence is indication-specific (Barth syndrome), and that does not equal proof for general cardiovascular prevention, aging, or "night owl damage" in otherwise healthy people.
What it is
Elamipretide is a mitochondria-targeting tetrapeptide that has been studied across mitochondrial and cardiovascular contexts and was granted FDA accelerated approval in September 2025 as Forzinity (elamipretide) injection for improving muscle strength in certain patients with Barth syndrome (a rare mitochondrial disease) weighing at least 30 kg.
Why it belongs here this week:
Night owl risk is mostly a behavior and timing problem. SS-31 is here as a reality check on how quickly people jump from "mitochondria are involved" to "there must be a mitochondria peptide solution." It is a serious drug in a narrow clinical lane, not a lifestyle tool – which makes it a perfect example of why we prioritize boring, measurable levers (light, timing, BP tracking) over biochemical wishful thinking.
This is squarely clinic / prescription / specialist territory, not a self-experiment block.
How it might work (mechanism – plausible, not settled)
What the literature suggests (in plain language):
Cardiolipin binding: Elamipretide is thought to interact with cardiolipin in the inner mitochondrial membrane, helping preserve membrane structure and function.
Mitochondrial bioenergetics support: It may improve efficiency of electron transport and ATP production in settings of mitochondrial dysfunction.
Reduced oxidative stress signaling: A recurring hypothesis is that stabilizing mitochondrial structure can reduce downstream oxidative damage and dysfunctional signaling.
Disease-context effect, not universal effect: Most of the compelling rationale comes from disease models or specific clinical populations, not from broad human prevention studies.
Mechanism expansion is ongoing: The 2025 MOA review emphasizes that mechanistic understanding has evolved beyond simplistic ROS-scavenging claims.
The evidence: claims vs reality
The claim (what people say):
"SS-31 is the mitochondrial peptide that fixes energy, heart function, and aging."
The reality check (what the literature supports):
That is too broad.
What is actually strong (or at least serious)
Regulatory / clinical credibility exists
FDA granted accelerated approval for Barth syndrome in 2025.
The approval explicitly states it is based on a measure considered reasonably likely to predict patient benefit (knee extensor muscle strength), and FDA requires a post-approval randomized confirmatory trial.
This is exactly the kind of nuance we want readers to understand: real signal, real uncertainty, real follow-up obligation.
Human trial evidence exists in specific populations
The TAZPOWER phase 2/3 randomized crossover trial plus open-label extension in genetically confirmed Barth syndrome provides the core human evidence base.
A phase 2/3 randomized clinical trial followed by an open-label extension to evaluate the effectiveness of elamipretide in Barth syndrome, a genetic disorder of mitochondrial cardiolipin metabolismA 2024 long-term open-label extension report describes sustained tolerability and improvements in functional/cardiac assessments in BTHS, but open-label data is not the same as definitive proof.
Long-term efficacy and safety of elamipretide in patients with Barth syndrome: 168-week open-label extension results of TAZPOWERThere is also older randomized heart failure work (single-infusion HFrEF study) showing safety/tolerability and short-term structural signals, but it was a small early-phase study and not a chronic-outcomes trial.
Novel Mitochondria-Targeting Peptide in Heart Failure Treatment: A Randomized, Placebo-Controlled Trial of Elamipretide
What is weaker than the internet claims suggest
General longevity / anti-aging use in healthy adults: not established.
Night owl heart-risk reduction: no direct evidence.
"Mitochondrial optimization" consumer framing: mostly extrapolation.
Cross-condition effect transfer: even if a drug helps in mitochondrial disease, that does not mean it should be generalized to prevention or wellness contexts.
This is where online peptide discourse often collapses important categories:
mechanistic plausibility
early clinical signal
approved indication
broad preventive use
Those are not the same thing.
Human vs preclinical summary (the practical version)
Human evidence: yes, but concentrated in Barth syndrome and selected disease studies
Preclinical evidence: extensive and mechanistically interesting
Generalizable prevention evidence: limited
Confidence for "mainstream healthy reader self-use": low
Decision rule (what to do instead this week)
If this section made you think, "I probably need to work on my mitochondria," your +1 for this week is not a peptide.
Do this instead:
Run the 14-day Night Owl Damage-Control Sprint
Track morning BP
Prioritize morning light + fixed wake time
Keep a 3-hour meal-to-bed gap on most nights
Audit late alcohol/nicotine
Re-test trend quality before adding anything expensive
That is less sexy than a peptide thread. It is also much more likely to improve your real-world risk profile.
Hard disclaimer (please read)
This section is educational only and is part of our research watchlist / clinic territory coverage. It is not medical advice.
Do not self-source peptides online. Do not use gray-market products, "research chemicals," or compounded products from unknown suppliers. Quality, identity, sterility, and dose accuracy are real risks.
Elamipretide/SS-31 is a drug-development / prescription-context topic, not a general wellness hack. If you have a medical condition involving mitochondrial disease, cardiomyopathy, or unexplained exercise intolerance, discuss evidence-based evaluation and treatment with a qualified clinician.
Hilo Band (affiliate partner)
If you are taking this week's protocol seriously, blood pressure trend quality matters more than one random reading.
Hilo is a blood pressure wearable system designed for ongoing tracking with an app-based trend view. In Europe, Hilo is described as a CE-marked Class IIa BP monitoring device, and the underlying Aktiia G0 system received FDA 510(k) clearance in the U.S. (K250415).
We just signed an affiliate deal, so if you buy through our link, we may earn a 10% commission (at no extra cost to you). We only want this in the newsletter when the tool is genuinely relevant to the experiment.
Important:
The Hilo Band and Hilo App are not diagnostic tools and should not be used as a substitute for professional medical advice or treatment. Always speak to your doctor about your results and never rely solely on this device for health decisions.
QUICK POLL
Which part of the Night Owl Damage-Control Sprint feels hardest right now?
QUOTE TO REMEMBER
💡 You do not need to become a different person this week. You just need a better system for your biology.
Closing Note
If you are a night owl, the goal is not perfection. The goal is less circadian friction: a consistent wake time, real morning light, fewer bright screens late, and a couple of measurable guardrails (like the 3-hour meal gap and BP trend).
Reply with your scoreboard after 7–14 days and tell me one thing:
What broke first – wake time, light, screens, meal timing, or the BP habit? I read every reply, and your patterns directly shape what we build next.
If this issue helped you reframe "night owl" from identity to strategy, forward it to one night person you care about.
Until next time,
Live longer. Upgrade wisely.
Rolf & the HEALTH HACK team
PS: If someone sent you this, you can subscribe here: Vitality Signals
Disclaimers
Educational only. This newsletter is not medical advice.
Talk to a qualified clinician before making major changes, especially if you have a medical condition or take prescription medications.
Do not delay or avoid medical care because of something you read here.
Peptide warning: do not self-source peptides online or use unverified products. Quality, contamination, sterility, and dose accuracy risks are real.

