
Hi {{ first name | there}},
Last week's poll leaned toward inflammatory tone, with oxidative stress load close behind. That fits this week's issue perfectly.
Most people still think of oral care in narrow terms: cleaner teeth, fresher breath, better appearance. The more interesting question is what chronic gum irritation and oral inflammation may be doing outside the mouth. That is where this gets more serious.
This week's issue is about a daily habit so ordinary that it rarely gets treated like a real health lever at all, even as the evidence starts pointing toward a bigger connection.
If this changes how you think about brushing, bleeding gums, or the bedtime clean-up routine, forward it to one person who still thinks oral care is mostly about white teeth.
Evidence-first health, delivered – and built.
Want the full Deep Dive? Upgrade to HEALTH HACK Pro and the Pro sections unlock on the web version right away.
-LONGEVITY PLAYBOOK-
The Mouth–Brain Inflammation Story Most People Miss

This is not really a toothpaste story. It is an inflammation story.
A new 2026 study in the Journal of Clinical Periodontology found that people who increased toothbrushing frequency to 3 or more times per day had lower risk of overall dementia and Alzheimer's disease during follow-up. A second 2026 cohort in Yonsei Medical Journal found that more frequent toothbrushing, brushing before sleep, and interdental cleaning were each associated with lower dementia risk, and the combination of brushing at least twice daily plus interdental cleaning showed the lowest risk profile in that analysis.
That does not mean "brush more and you are protected." It means your mouth now belongs on the brain-risk shortlist.
The real lever here is not mintier breath. It is less plaque, less gum inflammation, less bacterial spillover, and less chronic inflammatory noise. A 2025 scoping review concluded that the most plausible links between oral disease and Alzheimer's disease run through inflammation, oral dysbiosis, and downstream neuroinflammatory pathways.
That is what makes this more than an "interesting association."
The practical signal is clustering around three things:
brushing often enough
brushing before sleep
cleaning between the teeth, not just across them
The Yonsei paper also found a lower-risk signal for professional dental cleaning within the previous year. So the useful frame is not "be more dental." It is take oral inflammatory burden more seriously.
Oral health has quietly moved from "important but boring" to ignored but systemically relevant. The same broad logic that made people care more about visceral fat, insulin resistance, and sleep apnea applies here too: a chronic inflammatory burden does not become harmless merely by sitting in an unfashionable body region.
These are still mostly observational data, not randomized trials proving that brushing or flossing prevents dementia. The cohorts are largely Korean, healthier brushers may differ in other ways, and no one should pretend oral care cancels smoking, untreated sleep apnea, diabetes, hypertension, or inactivity. This is not a magic shield. It is a neglected lever.
It is also not a license to get aggressive. Brushing too hard, using hard bristles, or brushing immediately after acidic foods and drinks can backfire. The ADA advises waiting after acidic intake rather than brushing immediately, because enamel is temporarily softened.
So the honest takeaway is simple:
Do not think of the mouth as a cosmetic zone.
Think of it as a daily inflammation-control zone.
And if you have been treating bedtime brushing, between-teeth cleaning, dry mouth, or overdue dental care as "small stuff," this is the reminder: small stuff becomes big stuff when it repeats for years.
Unlock HEALTH HACK Pro for this week's decision-grade deep dive on the mouth–brain link – what the new studies actually found, what they do and do not prove, how much signal is real, where the overreach risk starts, and what deserves more serious attention right now.
THE MOVE
Run the 7-Night Mouth–Brain Reset
For the next 7 nights:
Brush gently before sleep
Clean between the teeth once
If you had something acidic, rinse first and wait before brushing
Do not finish the routine and then keep snacking
What to watch:
bleeding when cleaning between the teeth
morning "fuzzy teeth"
gum tenderness
bad breath on waking
dry mouth overnight
Safety / stop note: if bleeding keeps showing up, or you notice swelling, pain, loose teeth, recession, or pus, stop treating this like a self-optimization project and book a dentist.
Unlock HEALTH HACK Pro for the full 14-day Mouth–Brain Reset – the exact nightly sequence, the after-acid timing rule, the product-choice logic, the bleeding-gums decision tree, the dry-mouth fixes, and the stop rules that turn this from a nice idea into a real protocol.
-BIOMARKER OF THE WEEK-
Neutrophil-to-lymphocyte ratio (NLR)
NLR is a simple inflammation marker calculated from a standard complete blood count. It is not an oral-health test and not a dementia test. What makes it useful here is that it gives a rough read on background inflammatory tone without requiring a specialty panel.
A 2024 meta-analysis found higher NLR in periodontitis versus healthy controls, supporting the idea that gum disease is not just a local irritation story. A separate 2024 meta-analysis found higher NLR in Alzheimer's disease and mild cognitive impairment versus healthy controls, which makes it a reasonable bridge marker for an issue built around oral inflammation and brain risk.
How to measure it: from a routine CBC.
What "better" generally means: lower is usually better in the context of chronic inflammation – but only when read in context and not during an acute infection, recovery from illness, or another obvious inflammatory flare.
Useful frame: NLR is a trend marker, not a trophy marker. It is better for spotting whether inflammatory load looks broadly calm or broadly noisy than for making any mouth-specific conclusion.
Unlock HEALTH HACK Pro for the full NLR interpretation guide – when to test it, what can falsely push it up, what range shifts are actually interesting, how to read it next to oral inflammation, and when an "inflammation marker" is telling you almost nothing useful.
-MYTH OF THE WEEK-
"If you brush, the gaps do not matter."
Wrong.
This week's evidence did not point to brushing alone as the best pattern. The 2026 Yonsei Medical Journal cohort found a lower dementia-risk signal with the combination of regular toothbrushing plus interdental cleaning, and its figures show lower cumulative incidence in people using interdental cleaning devices.
That still does not mean interdental cleaning is a magic bullet or that the mouth–brain link is proven causal. It does mean this: toothbrushing alone likely leaves too much inflammatory territory untouched. And older evidence backs that up – interdental brushes used alongside toothbrushing remove more plaque than brushing alone, while a Cochrane review found that floss or interdental brushes added to brushing may reduce gingivitis or plaque more than brushing alone.
Safer replacement behavior: keep the brushing habit, then add one sustainable between-teeth method most nights. Not perfection. Not gadget collecting. Just a routine that reaches the places the toothbrush misses.
THE SUPPLEMENT
Oral Probiotic Lozenges
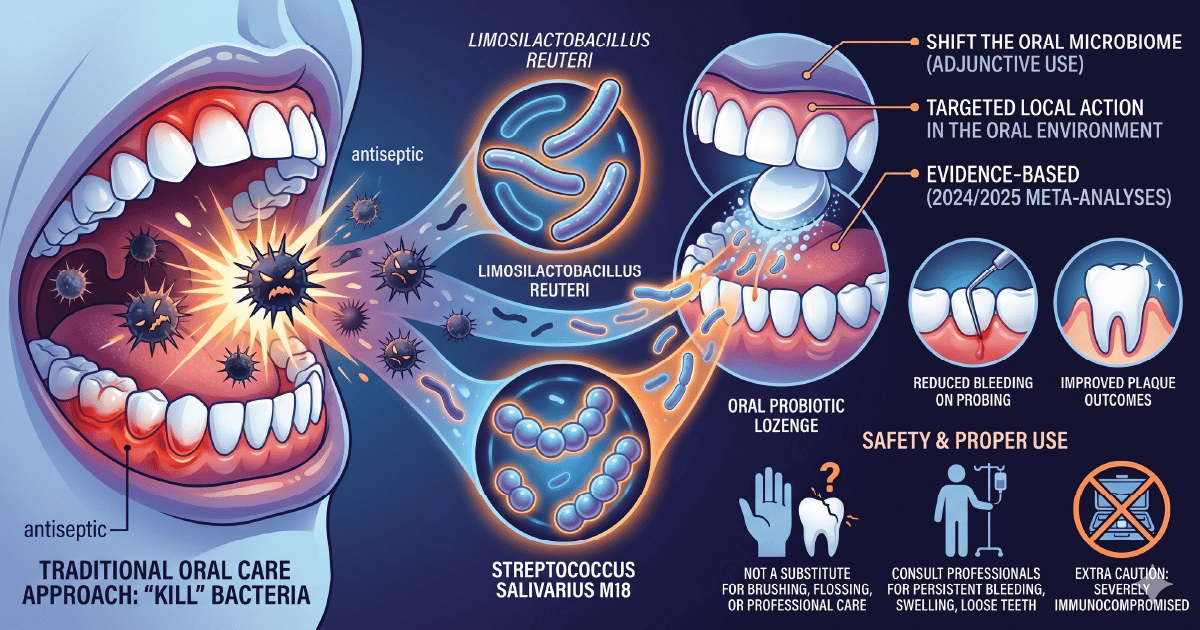
Most people hear "oral care" and think kill more bacteria.
The more interesting adjunct may be to shift the oral microbiome instead.
A 2025 systematic review and meta-analysis found that probiotics can be a useful adjunct in gingivitis and periodontitis, with benefits showing up most clearly in measures such as bleeding on probing and plaque-related outcomes. A 2024 network meta-analysis also identified Limosilactobacillus reuteri as one of the more promising adjunctive options in non-surgical periodontal therapy.
The honest framing is adjunct, not replacement.
This is not a substitute for brushing, cleaning between the teeth, or professional care when the gums are clearly telling you something is wrong. The best fit here is usually a lozenge or tablet aimed at the mouth rather than a generic swallowed capsule, since the target is the oral environment, not the gut.
The strain family that keeps showing up most often in this literature is L. reuteri. There is also newer trial-level interest in Streptococcus salivarius M18 lozenges, which improved periodontal measures in a 2025 randomized trial.
Safety note: extra caution if you are severely immunocompromised, and do not turn a persistent-bleeding, painful, swollen, or loose-tooth problem into a supplement experiment.
Unlock HEALTH HACK Pro for the oral-probiotic field guide – which strains have the best periodontal signal, lozenge vs capsule, when to use them, what they pair well with, what can backfire, and when this is the wrong move entirely.
-IN THE PRESS-
What we're reading
Coffee Is Not Just a Stimulant. It May Be a Microbiome Signal.
A new Nature Communications paper found that habitual coffee intake was linked to distinct gut-microbiome and metabolite patterns, and the study also reported differences in impulsivity, emotional reactivity, and memory between coffee drinkers and non-drinkers. One important caveat: this was a fairly small human study — 31 coffee drinkers vs 31 non-coffee drinkers, followed by abstinence and reintroduction phases — so this is more of a high-quality signal than a final verdict.
Nature
Midlife Hobbies May Matter More Than Alzheimer's Genes
A new report from Trinity College Dublin says that a diverse mix of social, physical, and intellectual activities in midlife was more strongly associated with cognition than the negative association of APOE e4, the best-known common genetic risk factor for late-onset Alzheimer's. The study looked at 700 cognitively healthy adults aged 40-59 and found that variety seemed to matter more than any single habit.
Neuroscience News
Creatine Still Looks Useful. Methylene Blue Still Looks Overhyped.
Scientific American did a nice job cutting through supplement noise here: creatine does have decent evidence for muscle support, while claims that adding methylene blue to the stack will help "body or brain" are described as way overblown. That makes this one a useful antidote to the current social-media stack culture.
Scientific American
Diet Drinks May Beat Sugar for Weight Control. Water Still Wins.
Harvard highlighted a new analysis from 3 prospective cohort studies covering 143,000 participants over a median 28 years. Replacing sugar-sweetened beverages with artificially sweetened beverages was associated with weight loss — but water was the best substitute for both.
Harvard Chan
Your Blood Pressure May Care About Salt in Your Water, Not Just Your Food
This one is surprisingly strong. A review summarized in ScienceAlert found that people exposed to saltier drinking water had about 3.22 mmHg higher systolic blood pressure, 2.82 mmHg higher diastolic blood pressure, and a 26% higher risk of hypertension, with the strongest associations in coastal populations.
ScienceAlert
-PEPTIDE OF THE WEEK-
LL-37 (host-defense peptide / clinic-watchlist)

LL-37 is exactly the kind of peptide that gets overhyped fast.
It sits at the intersection of antimicrobial defense, immune signaling, and tissue repair. That makes it sound like a universal fix. It is not. The real human evidence is much narrower than the internet version of the story. The clearest clinical signal is in topical wound-healing settings, not brain health, not general longevity, and not everyday "optimization."
What it is
LL-37 is the active human cathelicidin peptide involved in innate immune defense. It is relevant to antimicrobial activity, inflammatory signaling, and tissue repair, which is why it keeps showing up in conversations about wound healing and periodontal biology. A 2025 review on LL-37 in periodontitis summarizes that role clearly.
How it might work
Mechanistically, LL-37 can disrupt microbial membranes, recruit immune cells, and influence repair signaling.
That is the attractive part.
The less attractive part: context matters. A 2025 study of the LL-37 / FPR2 axis in periodontitis found higher expression in diseased gingival tissue and linked that signaling to clinical severity, with evidence that higher concentrations can amplify pro-inflammatory responses in inflamed gingival fibroblasts. In plain English: the biology is real, but it is not simple "more is better" biology.
The evidence: claims vs reality
There is real human evidence for LL-37.
It is just not the use-case most readers imagine.
The strongest clinical data are in topical venous-leg-ulcer studies, including randomized work and a phase IIb trial evaluating LL-37 in hard-to-heal venous leg ulcers. That is meaningful. It is also a long way from proving that LL-37 belongs in a consumer oral-health or brain-health routine.
The regulatory story changed this month as well. FDA’s April 2026 materials say cathelicidin LL-37 was removed from 503A Category 2 after the nomination was withdrawn, while FDA also says it plans to consult the PCAC about possible 503A bulks-list inclusion. At the same time, FDA’s safety-risk page says compounded LL-37 may pose immunogenicity risk for certain routes and may have peptide-related impurity / characterization issues. That makes LL-37 more relevant as a clinic-watchlist peptide. It does not make it casually safe.
Decision rule (what to do instead this week)
Do not chase LL-37.
Chase the lower-risk, better-supported lever from this week’s main issue: oral inflammatory burden.
That means better bedtime brushing, consistent between-teeth cleaning, attention to dry mouth, and escalation when the gums are clearly telling you something is wrong. The ordinary move has better consumer-level support than the sexy peptide.
Hard disclaimer (please read)
LL-37 is clinic / compounding territory. This section is educational only. Do not self-source peptides. Do not treat a change in FDA category status as a safety endorsement. Do not assume wound-healing data translate to oral, systemic, or brain-health self-use.
Unlock HEALTH HACK Pro for the LL-37 clinic-watchlist deep dive – where the human evidence is real, where the hype outruns the data, what the new FDA shift actually changes, and the exact clinician-level questions worth asking before anyone treats this like a routine peptide.
QUICK POLL
What is your biggest mouth–inflammation blind spot right now?
QUOTE TO REMEMBER
💡 Do not treat the mouth like a cosmetic zone. Treat it like an inflammation-control zone.
Closing Note
The most important health risks are not always the loudest ones.
Some sit in plain sight, repeat daily, and stay easy to dismiss right up until the bigger pattern comes into view.
That is the real point of this issue.
A small routine can still carry serious consequences when it touches chronic inflammation, daily exposure, and long time horizons.
If this week's issue changed how you think about brushing, bleeding gums, or bedtime oral care, forward it to one person who still thinks this is mostly about white teeth.
Until next time,
Live longer. Upgrade wisely.
Rolf & the HEALTH HACK team
PS: If someone sent you this, you can subscribe here: HEALTH HACK Newsletter
Disclaimer
Educational only. Not medical advice. Do not delay care. Consult your clinician for personal decisions – especially around symptoms, imaging, supplements, medications, or peptides. Do not self-source peptides.
