
Hi {{ first name | there}},
Last week's poll gave us an interesting signal: while 45.8% of you said "I'll do the 10-session Speed Block", and an additional 18.0% "I'll do it, but only if it's under 20 minutes", a meaningful 18.2% said the real problem is not cognition at all – it is sleep.
That matters. One of the most overlooked metabolic levers is not what you eat, but when your body is trying to sleep while you are still digesting. So this week, we are testing a simple rule that may improve both.
If this issue helps, forward it to one person who keeps trying harder diets when the timing of dinner might be the easier win. Subscribe here.
Evidence-first health, delivered – and built. (And yes, this kind of simple weekly scoreboard is exactly the kind of thing we are building into HEALTH HACK Pro.)
COMING SOON
In the coming months, we will introduce HEALTH HACK Pro - a deeper companion to HEALTH HACK for readers who want more structured implementation support.
Think: practical protocols, scoreboards, checklists, and decision tools that help turn evidence-first health ideas into weekly actions you can actually run (without hype, and without drowning in information).
We will send a separate email with details and an optional subscription link when it is ready - so you can decide if it is for you.
-LONGEVITY PLAYBOOK-
Stop Eating 3 Hours Before Bed, Not 3 Hours Earlier
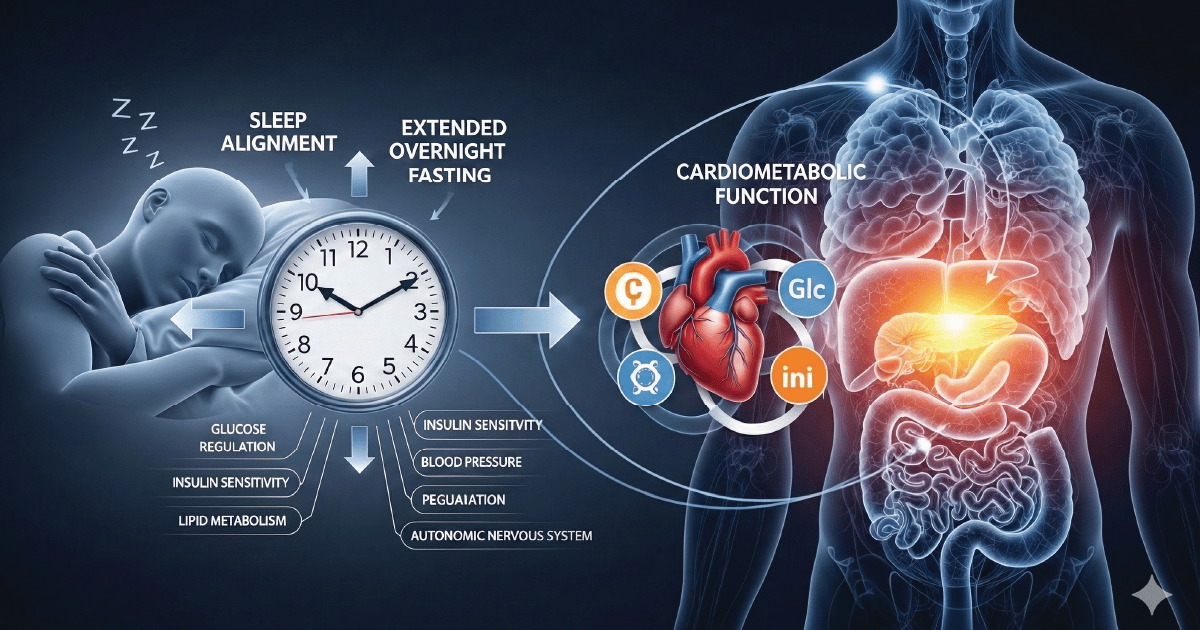
A new randomized study in Arteriosclerosis, Thrombosis, and Vascular Biology (AHA) tested a very practical idea: extend overnight fasting in a way that is aligned with sleep – specifically, no eating for the 3 hours before bedtime (plus dim lights before bed). The authors reported improved cardiometabolic function and stronger coordination between sleep/circadian regulation and autonomic/metabolic activity in middle-aged and older adults at higher cardiometabolic risk.
Study: Sleep-Aligned Extended Overnight Fasting Improves Nighttime and Daytime Cardiometabolic Function
The useful shift here is not "fast longer at all costs." It is: tie your fasting window to your sleep window. That matters because glucose tolerance, insulin sensitivity, autonomic tone, and melatonin/cortisol rhythms are all time-dependent. Earlier work on early time-restricted feeding also found benefits on insulin sensitivity and blood pressure even without weight loss, which supports the idea that timing has effects beyond calories alone.
Why now
Most people already know "eat less junk" and "move more." What they do not have is a decision rule they can run on a Tuesday night. "Kitchen closed 3 hours before bed" is one of those rare rules that is simple, measurable, and low-cost.
Mechanism – simplified
Late eating can collide with the body's nighttime physiology:
Glucose handling is often worse late in the biological day
Sleep can be affected by digestion, reflux, and body temperature
Autonomic "night dip" signals (heart rate, blood pressure) may be blunted when the body is still processing food
The new study is interesting because it looked at nighttime and daytime cardiometabolic function together – not just weight change.
Reality check (do not over-interpret this)
This was not a magic cure trial. It was a small study in a specific population (middle-aged/older adults with overweight/obesity and elevated cardiometabolic risk), and the protocol also included dimming lights before bed. That means you should not over-claim that "meal timing alone" explains 100% of the effect. It is better to think of this as a sleep-aligned behavior package worth testing safely.
Also, not every time-restricted eating study shows dramatic effects on every outcome. For example, a 2025 secondary analysis in JAMA Network Open found no significant differences in sleep, mood, or quality of life across different TRE timing schedules vs usual care in adults with overweight/obesity – which is useful because it keeps us honest and reminds us not to generalize one benefit to everything.
Study: Time-Restricted Eating and Sleep, Mood, and Quality of Life in Adults With Overweight or Obesity
THE PROTOCOL
3-3-13 Sleep-Aligned Fasting Trial (7 days)
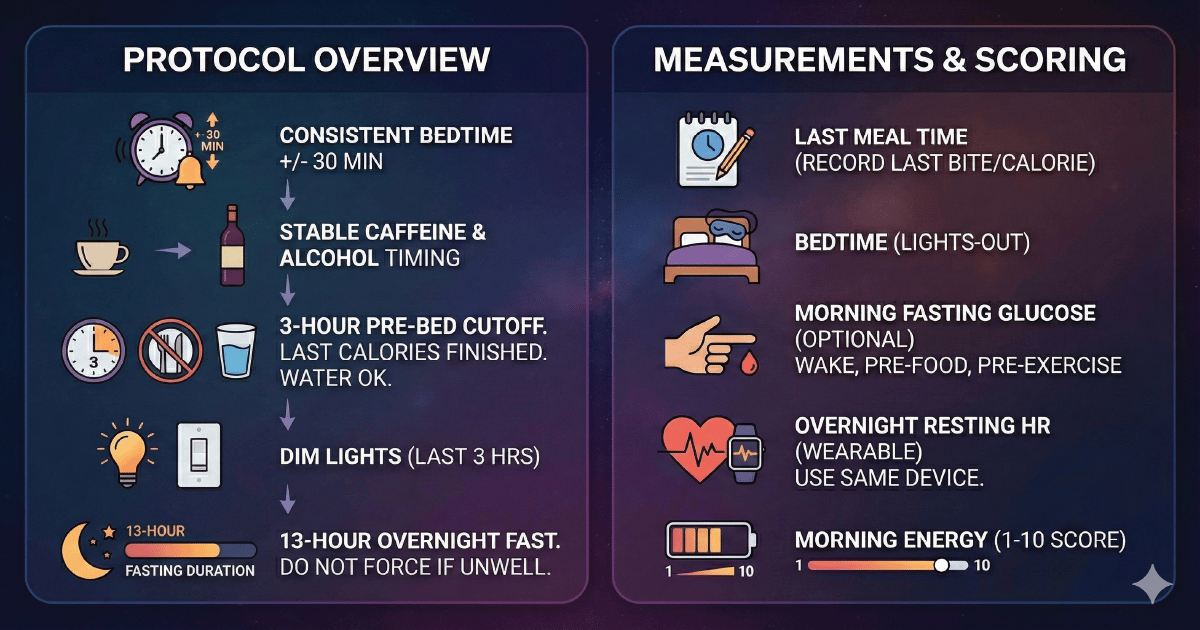
This is a doable experiment, not a forever rule.
Step-by-step
Pick your bedtime (target time) and keep it within +/-30 minutes.
Set a "kitchen closed" alarm for 3 hours before bed.
Finish your last calories by that cutoff. Water is fine.
Aim for a 13-hour overnight fast most days (do not force it if it makes you feel unwell).
Keep caffeine timing and alcohol intake as stable as possible this week.
If you can, dim lights in the last 3 hours before bed to reduce mixed signals. (This was part of the study context.)
Measurement instructions (simple, standardized)
Last meal time: record the time of your last bite/calorie
Bedtime: record lights-out time
Morning fasting glucose (optional but high signal): measure after waking, before food, before exercise (and ideally before coffee), after an overnight fast
Overnight resting HR (if wearable): use the same device all week
Morning energy: 1–10 score
Safety line (read this)
Do not run this if you have a history of an eating disorder, are pregnant/breastfeeding, are underweight, or you use glucose-lowering medication/insulin without clinician guidance. Stop and seek care if you get symptoms of hypoglycemia (shaking, sweating, confusion), severe dizziness, chest pain, fainting, or persistent reflux/vomiting.
TINY SCOREBOARD
Reply and paste this in:
Nights completed (3-hour cutoff): __ / 7
Average last meal -> bed gap: __ hours __ min
Morning energy (avg, 1–10): __
Fasting glucose change (if measured): __ -> __
What broke the streak most often: __
-BIOMARKER OF THE WEEK-
Fasting glucose (morning)
What it is:
Your blood glucose after an overnight fast. It is a simple snapshot of how your body is handling glucose in a fasting state.
How to measure:
Lab fasting plasma glucose (best for diagnosis/screening)
Or home glucometer/CGM for pattern tracking (not diagnosis)
CDC also provides a practical overview of what fasting blood sugar testing is and the standard category cutoffs. See CDC Diabetes Testing and CDC Manage Blood Sugar.
What "better" generally means:
For this week's experiment, "better" means more stable and/or lower morning fasting values over time (without hypoglycemia), in context with sleep and dinner timing. Do not obsess over one reading – look for a pattern across several days.
Why it matters:
Fasting glucose is not the whole story, but glucose dysregulation is linked to cardiometabolic risk, and even in people without diagnosed diabetes, fasting glucose levels are associated with vascular risk in a non-linear way.
-MYTH OF THE WEEK-
"If the fasting window is the same length, timing does not matter."
Why this is wrong:
The growing chrononutrition/TRE literature suggests timing can matter because metabolism is not constant across the day. The new sleep-aligned fasting trial specifically frames benefits around alignment with sleep and circadian/autonomic rhythms, and earlier eTRF work also showed cardiometabolic benefits beyond weight loss.
See this review on timing/circadian context: Time-restricted eating, the clock ticking behind the scenes
Safer replacement behavior (actionable):
Keep your fasting window reasonable, but anchor your first change to this rule: "Last calories >=3 hours before bed." Then measure for 7 days before changing anything else.
THE TOOL
Kitchen Close Alarm (plus one friction barrier)

This week's "tool" is deliberately boring: a phone alarm labeled "Kitchen closed – last calories now" set 3 hours before your target bedtime.
Why this works better than willpower alone:
Planning and cue-based behavior design (action planning, reminders, self-monitoring) consistently show up as useful behavior change components in health interventions. See the systematic review on planning interventions (PMC) and a reminder/implementation-intention mHealth study (PubMed, PMC).
Practical use (keep it boring and doable):
Alarm 1: "Last calories in 15 min"
Alarm 2 (optional): "Kitchen closed"
Add one friction barrier: clean the kitchen, turn off kitchen lights, or put snacks out of sight
Safety / contraindications:
If you have diabetes, are on glucose-lowering meds, or struggle with late-night hypoglycemia, discuss timing changes with your clinician before experimenting.
-SPONSORED-
The only clinically certified cuffless blood pressure monitor
Track your blood pressure continuously, day and night - without an inflatable cuff.
-IN THE PRESS-
What we're reading
Alcohol Profoundly Changes The Way Your Brain Communicates, Study Finds
A controlled human study (107 healthy adults) found that alcohol shifted resting brain networks toward more local processing and less global integration - and those network changes tracked how intoxicated people felt, not just breath alcohol levels. Interesting mechanism, but still a resting-state MRI study, not a life-behavior verdict.
ScienceAlert
Powerhouse athletes are actually prematurely aging their bodies thanks to an extreme exercise
The headline is loud, but the signal is worth watching: in 23 runners, longer ultra-endurance races were linked to stiffer red blood cells plus molecular signs of oxidative/inflammatory damage, with stronger effects at 171 km vs 40 km. Important caveat: small sample, pre/post sampling only, and long-term effects are still unknown.
New York Post
Japan approves world’s first regenerative medicines using iPS cells
A real milestone in regenerative medicine - Japan's health ministry panel approved commercialization of two iPS-cell-derived products, one for severe heart failure and one for Parkinson's disease. Not a consumer-health takeaway for this week, but a meaningful "the field is moving" signal.
South China Morning Post
Training harder could be rewiring your gut bacteria
In highly trained rowers, gut microbiome markers, SCFAs, stool frequency, and diet quality differed between high- and low-training-load phases. The useful nuance: this is probably not "exercise rewires your gut" in isolation - it looks more like training load + food quality + gut transit moving together.
ScienceDaily
Scientists Can Make Your Memory 'Young' Again – By Reprogramming Your Brain
An EPFL team reported that OSK-based partial reprogramming of memory-trace (engram) neurons restored learning and memory performance in aged and Alzheimer's-model mice. Scientifically exciting, but this is still targeted gene therapy in mice - not remotely a self-experiment or near-term prevention strategy.
Popular Mechanics
-PEPTIDE OF THE WEEK-
DSIP (delta sleep-inducing peptide, nonapeptide)
The sleep promise – and the evidence gap

DSIP is one of those peptides that keeps showing up whenever people go looking for "sleep peptides." It has an intriguing name, a long history, and just enough old human studies to create curiosity. It also has a major problem: the evidence base is old, mixed, and biologically unsettled. This is exactly why it belongs in a HEALTH HACK "research watchlist" block – not as a recommendation.
What it is
DSIP stands for delta sleep-inducing peptide, a short peptide (nonapeptide) first studied decades ago in the context of sleep regulation. Historically, it was investigated for possible effects on insomnia, sleep architecture, pain, stress, and endocrine signaling. Older reviews describe a surprisingly broad range of proposed effects, which is usually your cue to slow down and ask whether the biology is fully understood.
Start with the classic review and update:
Delta-sleep-inducing peptide (DSIP): a review
Delta-sleep-inducing peptide (DSIP): an update
Important context: DSIP is not a standard, mainstream, first-line insomnia treatment in major guideline-based sleep medicine. If you see it marketed online as if it were a proven sleep fix, that is already a red flag.
How it might work (mechanism – plausible, not settled)
What people propose (and what remains uncertain):
It may influence sleep architecture (especially slow-wave sleep) in some experimental contexts, which is where the name comes from.
It has been discussed as a modulator of neuroendocrine and stress-related pathways, but the precise physiological role in humans remains unclear.
Some preclinical work suggests interactions with pain and arousal systems, which could indirectly affect sleep initiation.
There may be DSIP-like immunoreactivity or related compounds that complicate interpretation of older findings, which is part of why the field remains unresolved.
Bottom line: there is enough biological plausibility to justify scientific interest, but not enough clarity to treat DSIP as a settled clinical tool.
The evidence: claims vs reality
The claim (what people say):
"DSIP improves sleep quality, deep sleep, and next-day recovery."
The reality check (what the literature supports):
The literature is mixed and largely old. Some early human studies reported improvements in sleep measures in insomniac patients, but later controlled analyses found the effects to be weak, inconsistent, or of limited clinical significance.
Human evidence (what exists)
There are older double-blind and crossover sleep-lab studies in chronic insomnia that are often cited:
One 1992 double-blind study found some improvements in objective sleep efficiency and sleep latency vs placebo, but the authors explicitly noted the statistically significant effects were weak and possibly partly explained by placebo-group changes.
Effects of delta sleep-inducing peptide on sleep of chronic insomniac patients. A double-blind studyA 1987 study in chronic insomniacs concluded that apparent differences were of little clinical significance once baseline differences were considered.
Study of delta sleep-inducing peptide efficacy in improving sleep on short-term administration to chronic insomniacsOther older reports and small series exist, but they are exactly the kind of evidence that can inflate confidence when read without modern standards in mind.
Preclinical / mechanistic evidence
Animal and mechanistic studies are one reason DSIP remains interesting in theory, especially around slow-wave sleep and stress/endocrine interactions. But preclinical signal does not equal reliable clinical effect in humans, especially for sleep where placebo effects, expectation, and protocol details matter a lot.
The biggest issue for HEALTH HACK readers
The strongest modern summary line is still the 2006 review calling DSIP a "still unresolved riddle" because its natural occurrence and biological activity remained obscure. That is not what a mature, clinically dependable evidence base sounds like.
Delta sleep-inducing peptide (DSIP): a still unresolved riddle
Decision rule (what to do instead this week)
If your real goal is better sleep and better next-day cardiometabolic rhythm, do this first:
Run the 7-day 3-3-13 sleep-aligned fasting trial (last calories >=3 hours before bed, ~13-hour overnight fast, stable bedtime, dim lights). This has a fresh randomized study behind it and gives you a measurable outcome this week. Start there before touching anything in peptide territory.
Hard disclaimer (please read)
Educational only. This section is a research watchlist, not a recommendation. DSIP is not a proven, mainstream insomnia treatment, and the evidence is mixed and dated. Do not self-source peptides online. Quality, identity, sterility, and contamination risks are real, and labeling is often unreliable. No dosing guidance here. If you have a sleep disorder, talk to a qualified sleep clinician and evaluate basics first (sleep apnea risk, caffeine/alcohol timing, light exposure, and medication effects).
QUICK POLL
Which part of this week's protocol feels hardest?
QUOTE TO REMEMBER
💡 You are not trying to "win" health in one heroic day – you are building a system your biology can run.
Closing Note
This week's experiment is intentionally simple. No optimization theater. No perfect macro math. Just one clear timing rule, tested consistently enough to learn something real from your own body. That is the point: not perfection, but signal.
If the week goes well, keep it. If it breaks, that is useful data too. Find the friction point (hunger, schedule, social dinners, late work) and adjust the system - not your self-respect.
A quick preview of what is coming: In the next months, we will introduce HEALTH HACK Pro - a deeper companion for readers who want more than ideas and want help with execution.
It will focus on implementation: practical protocol breakdowns, scoreboards, checklists, and simple decision tools to help turn trustworthy health science into weekly actions you can actually run.
When it is ready, we will send a separate email with the details and an optional subscription link, so you can decide if it is a fit for you.
Reply with your scoreboard after 7 days. I read those replies, and they help shape what we build next.
And if this issue helped clarify one practical rule, forward it to one person who is overcomplicating their evenings.
Until next time,
Live longer. Upgrade wisely.
Rolf & the HEALTH HACK team
PS: If someone sent you this, you can subscribe here: Vitality Signals

